Scientists Inject Viruses to Treat Woman’s Superbug‑Infected Wound
The viruses, called “bacteriophages,” may be a promising treatment option to kill superbugs more effectively.
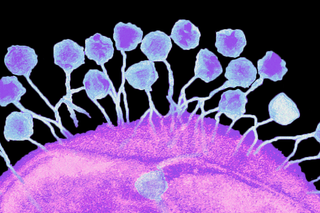
It may be time to move over Star Wars. “Microbe wars” could, perhaps, be the premise for the next science-fiction that captures our imagination in a world that has developed an interest in health-related science, courtesy of the global pandemic. This is a world where we have viruses doing the good work of slaying superbugs and protecting us — unlike the deadly coronavirus that is wreaking havoc across the world. Recently, scientists were able to use viruses to treat a woman’s infection after antibiotics failed to measure up to the task alone.
Published in Nature Communications this week, the report delves into the treatment of a 30-year-old woman injured by a suicide bombing at the Brussels airport; resulting in a “fracture-related pandrug-resistant Klebsiella pneumoniae infection.” She was treated with antibiotics for over 700 days — close to two years — but to no effect. Subsequently, the team of physicians treating her released viruses, called “bacteriophages,” into her wound using a catheter. In combination with antibiotics, the trick worked in a matter of days.
With the success of the experiment, scientists think bacteriophages, along with antibiotics, may be a promising treatment option to kill superbugs more effectively.
“Bacteriophage” — which literally means “bacteria eater” — refers to viruses that can infect bacteria. Called “phage therapy,” the route of treatment that uses them is still experimental since there aren’t any large-scale clinical trials to back it up yet.
Related on The Swaddle:
A Woman’s Immune System ‘Naturally’ Cured Her of HIV
In November 2016, the ethical board of the hospital where the woman was being treated gave its permission to try the therapy, and the woman’s consent was obtained too. However, due to a lack of consensus among the physicians treating her, the therapy finally began in February 2018.
“[T]he patient had been under various regimens of antibiotics but the femoral fracture was still not consolidated and the infection was persisting,” said Anaïs Eskenazi, a specialist in internal medicine and infectious disease in Brussels, Belgium, who is the first author of the study. “A few days after the treatment, the patient’s wound was already dry, and the skin was changing color from greyish to pink.”
Its success of phage therapy provides hope for a promising treatment option to kill superbugs, or antibiotic-resistant bacteria, more effectively. “I see this [experiment] as convincing evidence that you can get antibiotic and phage synergy,” said Paul Turner, a professor of ecology and evolutionary biology at Yale University, who wasn’t involved in the study. Turner believes there’s also potential for bacteriophages to be effective in isolation — and not just in combination with antibiotics, as in the present case — “especially if you’re going after pan-drug-resistant bacteria.”
Decades of overuse and even misuse of antibiotics have brought upon us antimicrobial resistance or AMR, which occurs when microbes evolve to become unresponsive to antimicrobial drugs. Since antibiotics cannot neutralize 100% of the bacteria within a prescribed course, the few bacteria that remain gradually evolve to resist the antibiotic. At the current rate, AMR bears the potential to become the “next global pandemic,” and has already been declared among the 10 biggest threats to global public health by the World Health Organization (WHO).
Related on The Swaddle:
Rising Pollution in the Ganges May Lead to Neurological Diseases: Study
Unfortunately, India is among the worst affected by the problem and contributes to one-fourth of the global burden of multidrug-resistant tuberculosis. According to Dr. Sumanth Gandra, an epidemiologist and associate professor of medicine at the Barnes-Jewish Hospital in the U.S., who wasn’t involved in the present study, India is the “largest consumer of antibiotics in the world” and a “poster child for antibiotic misuse in low- and middle-income countries.” And the global pandemic worsened the situation — not only were patients prescribed antibiotics due to a lack of clarity on how to treat Covid19, but people also self-medicated with the drugs.
However, its impact will not be restricted to India alone. “Bacteria that have become resistant to antibiotics don’t have boundaries. They can spread to any person in any country,” Gandra had warned in July.
So, phage therapy, which certainly bears promise for healthcare in India, has the potential to revolutionize treatments of superbugs globally — but based on data obtained through large-scale clinical trials, not just isolated experiments. As Turner noted, “This is just the gold-standard… phages have to be held up to the same gold standard.”
“The concept of using viruses to kill bacteria first emerged more than a century ago… However, scientists’ understanding of phages was limited at the time, and following the discovery and pharmaceutical production of antibiotics, the field was largely abandoned,” an article on Live Science explains, adding that “interest in phage therapy resurfaced within the last decade, as scientists began searching for new strategies to take down antibiotic-resistant superbugs.”
Well, better late than never. And the viruses certainly seem to be “slayin’ it” — how often is that something we get to say about microbes, especially in a positive sense?
Devrupa Rakshit is an Associate Editor at The Swaddle. She is a lawyer by education, a poet by accident, a painter by shaukh, and autistic by birth. You can find her on Instagram @devruparakshit.
Related


64% of Covid19 Vaccine Side‑Effects Are Not Due to Vaccines, but the ‘Nocebo Effect’: Study