
Banning Blood Donation Based on Sexual Orientation or Practices Is Unfair and Ineffective
Technology can make blood donation safer and more equitable for both donors and recipients.
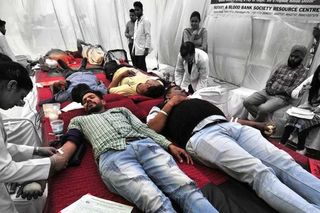
A well-functioning national blood system requires a pool of safe and voluntary donors. In 2017, India’s National Blood Transfusion Council (NBTC) approved the first-ever uniform guidelines for blood donor screening and selection. Ideally, if a donor matches the selection criteria laid down in these guidelines, blood banks will accept their blood. In cases in which donations might prove risky to the recipient or the donor themselves, the guidelines suggest deferring their donations for some months or permanently. This is primarily based on the precautionary principle in order to protect the interest of the blood recipient.
These guidelines suggest permanent deferral (lifelong bans) on donations by populations at risk for HIV infections. This includes “transgenders, men who have sex with men (MSM), female sex workers, injecting drug users, and persons with multiple sex partners.” This means that donor screening questionnaires in blood banks now require male donors to share details of their sexual behavior, especially their male-to-male sexual activity.
The issue is these lifetime blood donor bans are ineffective in securing safe and infection-free blood for patients needing transfusions. They are discriminatory toward those banned and they inhibit the collection of readily available blood that India sorely needs. Luckily, technology offers a way to solve these problems and make blood donation more equitable for both donors and recipients.
Efficacy of blood donor bans
Blood donor screening is a multi-layered process comprising donor questionnaires and counseling, followed by mandatory screening tests for transfusion-transmitted infections like HIV, hepatitis B, hepatitis C, syphilis and malaria.
Donor selection and screening are usually the only two steps followed in low-resource settings, such as in India. But these are only gatekeepers in safe blood stewardship, not fail-safes. Social stigma and taboo might be inhibiting factors for persons to honestly reveal their past sexual behaviors. However, a bigger factor for dishonest self-reporting is replacement donation, which is more or less unique to India. Simply put, friends and kin of patients in need of transfusions are coerced by blood banks to donate an equivalent number of units as a replacement for those used by the patient. In a situation where blood is critical to medical treatment of their family, replacement donors simply hide details or lie to donate their blood.
As a result, the National AIDS Control Organization’s (NACO) response to an RTI revealed that 1,342 people across India contracted an HIV infection through blood transfusions between 2018 and 2019, even after NBTC’s explicit guidelines. These bans don’t work.
Related on The Swaddle:
Private Cord Blood Banking Is Mostly Ineffective, Says IAP
Global experience of blood donor bans
The permanent ban on blood donation by stigmatized communities, such as India’s, has been criticized worldwide as being selectively discriminatory and lacking rigorous scientific justification. In recent years, bodies like the European Union and the World Health Organization have modified their guidelines to introduce the term “risky sexual behavior” without any reference to the sexual orientation or practices, or occupation of the donor. In fact, WHO guidelines for donor selection call for review or revaluation of deferral criteria taking into account changes in disease epidemiology, available technologies, and on-going research; for instance, changes in HIV/AIDS epidemiology mean MSM populations aren’t the focal point of control efforts in many countries anymore and therefore are no longer the likeliest to pass on an infection via blood donation.
Most nations have now reassessed lifetime blood donor bans in favor of shorter deferrals for MSM and transgender people (for instance, 1 year in the U.S. and 3 months in Canada and the U.K.). Some countries have followed an individual risk-assessment approach instead of a time-based exclusion. Argentina, Spain, Italy, and South Africa, for instance, assess both men and women on their sexual risk and make eligibility determinations.
Mathematical modeling studies from the U.K. and Canada show that reducing deferral periods to 1 year would have a marginal risk (approximately one extra HIV infection every 455 years) of increasing HIV transmission. Some initial studieseven show that relaxing deferrals can improve donor compliance to donation criteria and honest self-reporting, which may paradoxically reduce the risk of an HIV-positive donation entering the blood supply. Such estimations have not yet been conducted in India.
Globally, the movement for ending these bans also comes from the potential increase in blood supply that these populations could bring. An estimation from the U.S. suggested that lifting lifetime blood donor bans on certain communities could increase the supply by 2% to 4%. This is a critical factor for India, where the blood shortage stands at approximately 15%.
Related on The Swaddle:
What a Transgender‑Friendly Health Care System Would Look Like
Technology as the disrupter
When these bans were first implemented in the 1980s, an HIV test would not be able to detect the infection until about six to 14 weeks after contracting it. This allowed a window wherein an infected person might not know they were infected, during which they might donate blood. The tests available at that time were also highly inaccurate, leaving a chance of one HIV infection per every 153.123 units of blood.
However, with the new arsenal of cutting-edge screening technologies that blood banks (at least bigger ones) have, there could be nearly 100% accuracy in detection, reducing the risk of HIV-contaminated blood infection to 1 per 8 to 12 million donations.
This is the third, fail-safe step in safe blood stewardship: pathogen reduction, which is essential and increasingly accessible. Pathogen Reduction Technologies (PRT) are capable of clearing blood of all its pathogens post-collection and are touted as the holy grail of blood safety. If there is any risk posed by less-stringent deferral norms for men who have sex with men, transgender people, female sex workers, and others, PRT can potentially mitigate the risk completely, or at least substantially, in post-screening treatment of blood.
Countries like Belgium and Switzerland have long committed to using PRT on every single unit of blood collected in order to achieve the highest standards in blood safety and protect patient interests. In India, however, PRT is nascent. Even advanced tests like NAT and ELISA, which have higher sensitivity and accuracy in detecting infections, are used only in very advanced blood banks and their high cost is pawned off to the patients.
The high fixed cost of technologies, coupled with ceilings on blood processing charges, leave blood establishments with little ability to experiment with technology. Regulators and policymakers argue that fringe blood establishments in far-flung and rural areas cannot implement advanced testing. This argument doesn’t acknowledge the role of the government as an enabler. State funding is needed for the implementation of advanced technologies in public and patient interest. That’s how universal PRT commitments in Belgium and Switzerland worked out — the government stepped in.
Application of PRT can begin in advanced health facilities that can serve as hubs for centralized blood processing from satellite blood collection facilities (or spokes). But as this begins, so too must bans on donations from stigmatized communities be overhauled. Instead of a blanket ban, individual blood banks can carry out their own risk assessments depending upon their technological capacity.
NBTC’s guidelines are derived from a legacy of fear rather than scientific fact and only serve to be blatantly discriminatory. In the wake of the constitutional recognition of LGBTQIA+ rights, restrictions like these should also fall at the anvil of India’s sprawling jurisprudence of equality.
Shorter deferrals can be explored but it is nothing more than a piecemeal negotiation to decide the extent of exclusion. Ending exclusion requires moving towards an individual and gender-blind risk-assessment, and the use of technology. After all, stereotypes cannot be gift-wrapped as a precaution, and the cost of enabling technologies cannot win the trade-off against the emotional burden of discrimination.
Abhinav Verma is a lawyer and public policy consultant in health and technology.
Related


Female Health Experts Lack the Twitter Influence of Their Male Peers, Study Finds
